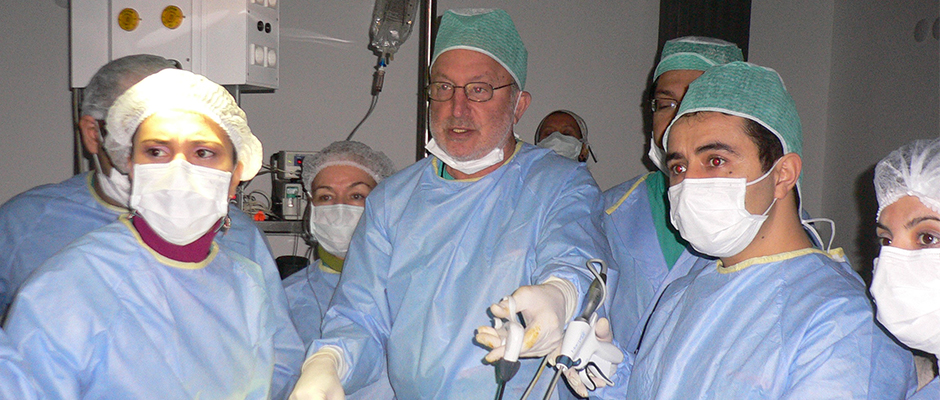
Above, Dr. Harry Reich (center), performs a laparoscopic excision surgery as his surgical team looks on.
Do you have a burning question for EndoFound’s Honorary Medical Director Emeritus and Senior Medical Advisor, Dr. Harry Reich? E-mail him at harry@endofound.org or visit EndoFound’s official Instagram, Facebook or Twitter, tag us and ask a question with the hashtag #askharry, and you could see your answer featured here!
I would like to comment on some criticism I received from the last article I wrote about the CO2 laser. Please realize that these columns are written from my own personal experience. As I am retired, I try to be objective and not write for anyone else. Just my views.
I have nothing but admiration for Dr. Ken Sinervo and in no way did I consciously demean his expertise with the carbon dioxide laser to excise endometriosis.
Now, on to the ovary, to address some of the criticism I received, and also to lay down some basic ground rules to treat ovarian endometriosis. In my column, I explained that if you have an endometrioma or an endometriosis-filled ovarian cyst, you don’t want to use any form of heat source inside the ovaries to excise it, because doing so can cause damage to the eggs. I will stand by that statement, and that includes the use of any heat source, including electrosurgery and any type of laser.
Endometriosis can be present as small deposits on the surface of the ovary. More commonly, endometriosis is also present on the pelvic sidewall. Endometriomas occur when the ovary opens up during ovulation, and the endometriosis from the pelvic sidewall gets inside the ovary.
The ovary and the endometrioma inside have two distinct layers with a plane in between. Think of that plane as a solid foundation of a home, with a parasite getting into it.
These endometriomas, or chocolate cysts, have been treated by excision surgery for many years, certainly before my residency training in the early 70s. The excision was done through a bikini line-wide cut, or laparotomy until the late 70’s when I began excising them by laparoscopy, which is minimally invasive. (I was actually the very first doctor in the United States to use this method to remove endometriomas.)
Below, an animation shows how an endometrioma forms inside of the ovary
While superficial endometriosis on the surface of the ovary can be vaporized with electrosurgery through a needle electrode or CO2 laser, the principles of excision of an endometrioma by laparotomy or laparoscopy are the same: the best way to get rid of an endometrioma is to excise it.
Now, I want you to imagine yourself peeling an orange.
The object of surgery is to remove 100 percent of that endometrioma. If you don't take it all out, it keeps growing back—but it shouldn't! The problem most doctors have is, they're not dissecting underneath and outside of the ovary on the pelvic sidewall where the endometriosis originates.
I also believe that 90 percent of endo surgeons are not going to peel off the cyst inside of the ovary painstakingly. Instead, they'll hastily try to deactivate the endometriosis in the cyst by using laser or electrosurgery. But, again, the way to get rid of the cyst is excise it, just like taking off that orange rind and removing the juicy, orange flesh inside. Only with the ovary, that "rind" usually falls back together on its own with minimal bleeding. That peeling and separating motion in removing the endometrioma is what we call mechanical energy; traction or counter-traction; or good old-fashioned elbow grease. That's what you need so that you won't damage the eggs.
With this method, minimal bleeding usually stops spontaneously.
@endowarriorgoddess asks: H
It's a fancy term for inflammation. It can indicate blockage of the fallopian tubes. It's more of a pathological term, not a clinical term. It's a term used by the people who analyze the tissue removed during surgery, under a microscope after surgery. If your tubes are blocked, and you desire to conceive, you may consider IVF to bypass the blockage.
Editor’s note: The opinions, beliefs, and viewpoints expressed by Dr. Harry Reich in this column are solely his own and based on his experience.







