What is painful sex?
The third predominant symptom of endometriosis is painful sex (dyspareunia). Patients with endometriosis often find themselves experiencing physical pain when engaging in sex, which is a very personal note for patients to express to their gynecologist. Nevertheless, it must be taken into account as it can help determine the level of pain and the anatomical location to which endometriosis lesions are located.
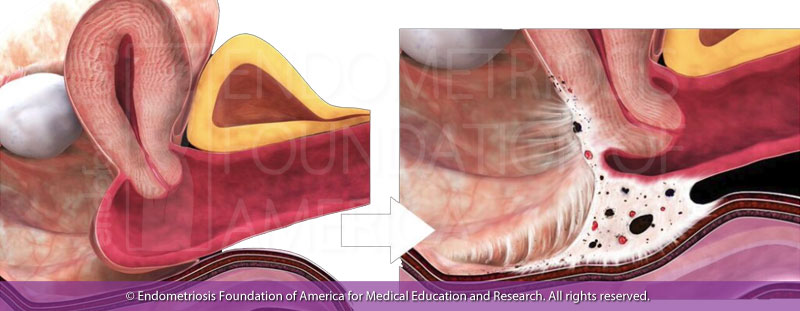
How does endometriosis cause pain during sex?
The area behind the uterus is called the cul-de-sac, or Pouch of Douglas. Normally it is lined by the smooth peritoneum, the skin-like sheet of tissue that covers the uterus and vagina anteriorly (in front), and the rectum posteriorly (in back), keeping the rectum, vagina, and uterus free from each other. Endometriosis will frequently adhere the vagina to the rectum. The pain caused by endometriosis during sex is deep; it comes from the inflammation and fibrosis fusing the front wall of the rectum to the back wall of the vagina. Mobility and expansion of the upper posterior vagina behind the cervix normally occurs during sex, but not if endometriosis is present. The pain can be more intense in certain sexual positions than in others, depending on exactly where the endometriosis is located and how advanced it is. If it is widespread, pain may be present no matter the position.
The care needed to discuss painful sex
Painful sex is a very personal matter and it can be extremely difficult to discuss the physical challenges experienced during sex. When a patient visits the doctor and discusses their symptoms, it’s rare to voluntarily mention painful sex as being one of them. Nevertheless, it is an important fact to disclose, not only for the good of her physical health, but also because the symptom is one that can cause tension in, or even break up, a relationship.
Surgery for painful sex
Laparoscopic excision of endometriosis is the gold standard for conservative surgical treatment. However, in cases of painful sex, it is important to specify that there must be a focus on endometriosis infiltrating the anterior and posterior cul-de-sac. By focusing on these areas, studies have found that upon removal of the endometriosis through excision surgery, patients experience improvements in dyspareunia symptoms as well as the quality of their sex life. It is, therefore, crucial to discuss these types of findings when choosing a doctor if a patient decides that surgical excision is the right treatment option.
Other ways of managing painful sex
While dealing with painful sex can be highly difficult, there are ways and tips to keep in mind in order to find relief in this constant struggle, such as:
-
Communication: Sex is meant to be a pleasant experience between two people who care for one another. Therefore, it is important to be vocal to your provider and your partner about your symptoms.
-
The timing of sex: Many individuals who experience dyspareunia due to endometriosis find that their pain varies depending on the timing of their menstrual cycle, and this is no coincidence as pain can be aggravated during the period. Some couples find relief by not engaging in sex during menstruation.
-
Other forms of intimacy: Couples have found relief from dyspareunia symptoms by engaging in other forms of intimacy, especially during the period. Sex is not the only way to find pleasure in the bedroom. Other forms of pleasure include oral sex, mutual masturbation, etc.
The danger in "tolerating" the pain
Often, patients experiencing pain during sex will not complain as they may not want to interrupt intimacy with their partner. However, it is important for patients to know that dyspareunia is a real symptom of the disease that must be taken into account and resolved.
A partner’s role in cases of painful sex
From the partner’s perspective, it may be difficult to know the pain that their loved one is experiencing, especially if communication about dyspareunia is not present within the relationship. Even a couple who has had a strong relationship for several years can face struggles if the disease causes the frequency of sex to diminish. This is another reason why diagnosing and treating endometriosis early is so important. Nobody wants it to reach a stage in which it is affecting the patient’s intimate relationship. For men and women whose partners are suffering from endometriosis, it is thus crucial to support their loved one. This means being mindful and listening to your partner if they say they are in pain. It can also mean accompanying them to gynecologist appointments. Endometriosis experts recommend couples coming in together as the partner of the patient suffering may have a keen insight into the patient’s symptoms.
References
-
S. Ferrero et al., "Deep dyspareunia and sex life after laparoscopic excision of endometriosis." Human Reproduction, Volume 22, Issue 4, 1 April 2007 p. 1142-1148.
-
Paul J. Yong et al., "Anatomic sites and associated clinical factors for deep dyspareunia." The International Society for Sexual Medicine. September 2017 Volume 5, Issue 3, Pages e184-e195.
-
Endometriosis and Painful Sex (Dyspareunia), drseckin.com

